Predictive factors for 90 day mortality in stage III NSCLC patients treated with chemo-radiotherapy
Maarten Lambrecht,
Belgium
PO-1247
Abstract
Predictive factors for 90 day mortality in stage III NSCLC patients treated with chemo-radiotherapy
Authors: Maarten Lambrecht1, Anne-Sophie Van de Velde1, Saartje Verfaillie2, Gilles Defraene3, Patrick Berkovic1, Christophe Dooms2, Johan Vansteenkiste2, Els Wauters2
1UZ Leuven Gasthuisberg, Radiation Oncology, Leuven, Belgium; 2UZ Leuven Gasthuisberg, Pneumology, Leuven, Belgium; 3KULeuven, Laboratory of Experimental Radiotherapy, Leuven, Belgium
Show Affiliations
Hide Affiliations
Purpose or Objective
Considering
the different co-morbidities of the patients and the potential toxicities of
combined chemo- and radiotherapy when treating stage III unresectable non-small
cell lung cancer (NSCLC), early mortality rates are a concern. With this study our
aim was to assess the 90 day mortality of the stage III NSCLC patients treated
at our center, and explore predictive factors.
Material and Methods
Consecutive patients were included who commenced concurrent or
sequential chemoradiotherapy between 04-2011 and 06-2018. Baseline clinical
case-mix variables (age, performance status, pack years, T-stage, pathology,
N-stage, charlson comorbidity Index (CCI) and baseline pulmonary function) and
treatment-related variables (number of chemotherapy cycles, sequential vs
concurrent chemotherapy, fractionation dose, overall treatment time, tumor
volume heart V5, V20, V50, mean heart dose, Lung V5 and mean lung dose) were retrieved.
The 90 day mortality was calculated from the last day of radiotherapy to the
date of death. Univariable logistic regression was performed for all
clinical case-mix and treatment related factor. Multivariable logistic
regression was performed with the uncorrelated (r<0.6) variables that had a
univariable p<0.1 (age, sequential vs concurrent, performance status, Lung
V5).
Results
A total of
148 patient were included in this preliminary analysis. Ninety days mortality
in this population was 8.8%. Univariable
analysis of all factors are depicted in table 1.
After
multivariable analysis performance status remained significantly associated with 90 day
mortality after radical chemo-radiotherapy (p=0.003, OR=0.85 (0.77; 0.95)),
while the lung V5 remained borderline correlated (p=0.08, OR 1.040
(0.995;1.095)). Sequential versus concurrent chemotherapy and age were no
longer significant.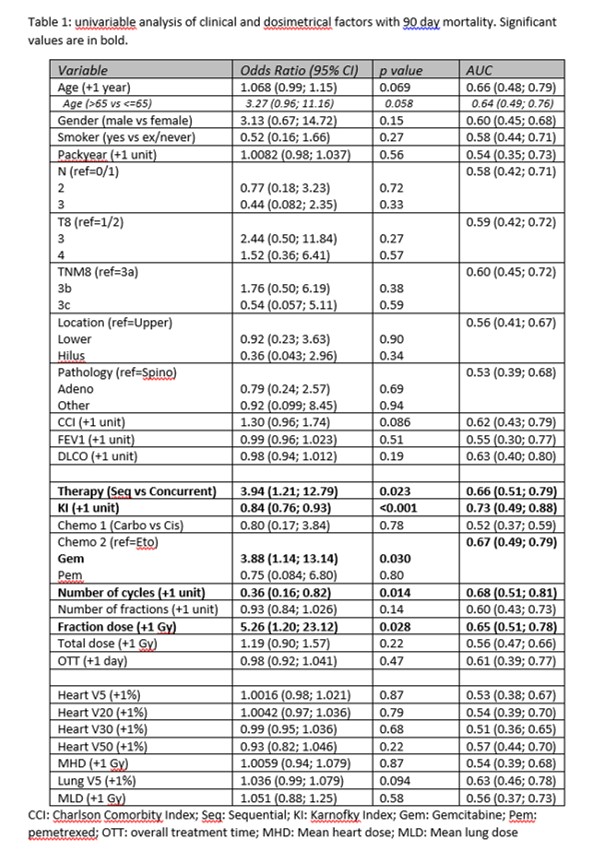
Conclusion
The initial
performance status seems to be the most important predictor of 90 day mortality
after chemoradiotherapy. A larger dataset will be constructed to further
analyze the influence of the lung V5 on early mortality.