Dose constraints validation in moderate hypofractionation in localized prostate cancer
PO-1356
Abstract
Dose constraints validation in moderate hypofractionation in localized prostate cancer
Authors: Xavier Maldonado1, Manuel Altabas1, Josep Garre1, Miriam Vazquez1, Susana Magriña1, Alba Delgado1, Noelia Docampo1, André Geng1, Marcelino Hermida2, David Sanchez-Artuño2, Jordi Giralt1
1HU Vall d'Hebron, Radiation Oncology, Barcelona, Spain; 2HU Vall d'Hebron, Physics, Barcelona, Spain
Show Affiliations
Hide Affiliations
Purpose or Objective
In September 2019 our department adopted the
CHIPP hypofractionated scheme for the treatment of localized prostate cancer.
We have assessed and compared the acute toxicity to validate the new critical
organ dose constraints designed in terms of isotoxicity when moving from
conventional to moderate hypofractionation.
Material and Methods
Acute
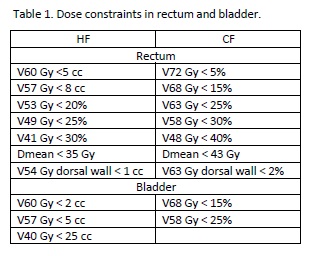
toxicity (graded according to CTCAE 4.0) from 40 men with localized prostate
cancer (T1-T3N0M0) treated with moderate hypofractionation schedule (HF) (60-62
Gy in 20 fractions over 4 weeks) and adapted dose constraints (Table 1) is
compared to a retrospective paired sample (n=42) treated with conventional
fractionation (CF) regime (72 Gy in 30 fractions over 6 weeks). PTV design was
comparable as well as the use of androgen deprivation. Both populations were
treated by Halcyon Accelerator or True Beam Linac with a VMAT technique. Daily
CBCT or fiducial marker triggered with KV images was used as IGRT method. Acute
data were prospectively collected using physician/nurse questionnaires:
baseline, weekly the first 6 weeks and monthly from the end of treatment. The χ²
test and t-student test were used to compare baseline characteristics of the
two populations and the overall worst degree of toxicity.
Results
When comparing the two populations,
median age was 74 years old (p=0,24), median Corporal mass index 35 (p=0.39),
30% presented diabetes(p=0.9), 24% on oral anticoagulants (p=0.36). ISUP was
grade 2/3 in 71% of patients (p=0.61), median PSA 11 ng/ml (p=0,2). Use of ADT
for 6 month in 35% and 24 month in 33% (p=0,75). IPSS score 0-7 in 50,6% and 8-19 in 49,4%
(p=0,53). There weren’t statistical differences in patients characteristics
between populations except for tobacco use (23% in CF and 0% in HF, p=0.001), median
Charlson score (0-5 73% in CF and 45% in HF, p=0.013) and clinical T (T1 78% in
CF and 21% in HF, p=0,024). When the T stage was mpMR assessed there was no
difference (4% and 5% for CF and HF respectively). Main acute GU and GI
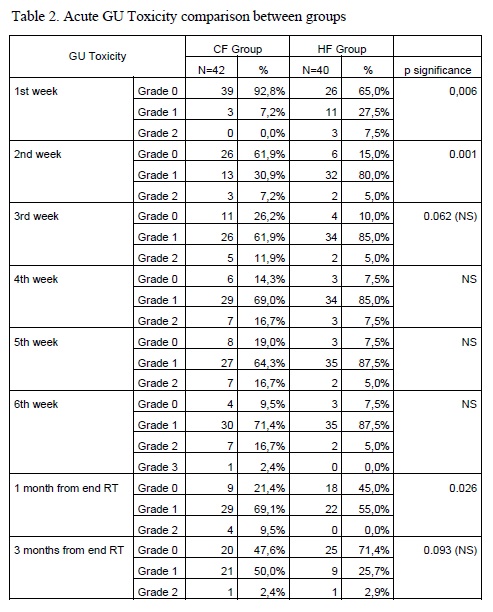
toxicity were grade 0-1 with no grade 3-4. Acute GU toxicity from week 1 to 6,
at 1 month and at 3 month is displayed in Table 2. There were statistical
differences in weeks 1 and 2, against HF and at 1 month against CF. Acute G2 GU
toxicity was more frequent in CF (10%) than in HF (4,7%) (p=NS). Regarding
acute GI toxicity it has been mild with no grade 2, 3 or 4. There were neither
differences comparing groups nor during the follow up at 1 or 3 month (0 vs 7%
and 0 vs 2%, p= 0.25).
Conclusion
We have validated our new critical organ constraints
regarding acute toxicity in terms of isotoxicity. Acute GU toxicity appears
earlier in HF group but recovers faster, without differences in grade but with
a higher G2 tendency in the CF group. GI acute toxicity has been mild with no
differences between arms.