Does intra-fraction motion of pelvic lymph nodes depend on localisation in online MR-guided RT?
M.V. Noordeloos, K. Antonissen, K. Ezendam, E. Bongers, P.M. Jeene and D. Schuring
ESTRO 2024 Congress report
Objective
Since June 2021, we have been performing stereotactic body radiotherapy for lymph-node oligometastases through the use of online adaptive magnetic resonance (MR)-guided adaptive radiotherapy (MRgART) on a 1.5T MR-Linac. This treatment offers the possibility of online plan adaptation. Mobility of the nodes may vary, depending on their location. The primary objective of this study was to quantify the intrafraction motion of lymph-node oligometastases during the online treatment procedure and to correlate this with their location. The secondary objective was to calculate optimal planning target volume (PTV) margins for each location.
Material/Methods
From June 2021 until April 2024, 66 patients with pelvic lymph-node oligometastases were treated on a 1.5T MR-Linac (Elekta Unity, Crawley, UK) with a prescription dose of 5x7Gy to the PTV, aiming to escalate the dose in the clinical target volume (CTV). Daily MRgART was performed through the application of an adapt-to-shape (ATS) workflow, in which the CTV is rigidly copied to and translated onto the MR that had been acquired at the start of treatment (session scan). Nearby organs at risk were recontoured. The treatment plan was adapted based on daily anatomy. A position verification MR (pulmonary vein scan) was acquired just prior to treatment, to verify that the node remained within the PTV. During beam delivery, the node was monitored through the use of cine-MR in transversal, sagittal and coronal directions. After treatment, a third MR (post-scan) was acquired. Intrafraction motion was quantified by registering the post-scan on the session MR. The shift in lateral, longitudinal and anterior-posterior directions, as well as the 3D displacement, was recorded. Each lymph node was classified as a mesorectal, para-aortic, para-iliac, or obturator node. Pairwise statistical testing was performed to investigate whether there were any significant differences in intrafraction motion for the different node localisations. Finally, the percentage of fractions with an intrafraction motion that exceeded a PTV margin of 1mm, 2mm, or 3mm was determined for each localisation.
Results
In total, 66 patients with 92 lymph nodes were treated with five fractions each, resulting in 460 registrations. Of these nodes, 17 were located in the mesorectum, 13 were para-aortic nodes, 29 para-iliac, and 33 obturator nodes. The measured intrafraction motion in the lateral, longitudinal and anterior-posterior directions, and the 3D displacement, were visualised in a box-and-whisker plot (Figure 1). A statistically significant difference in the intrafraction motion was observed for the mesorectal nodes, compared with the other locations for the anterior-posterior direction, as well as the 3D displacement. No statistically significant differences were found among the other locations, or in other directions.
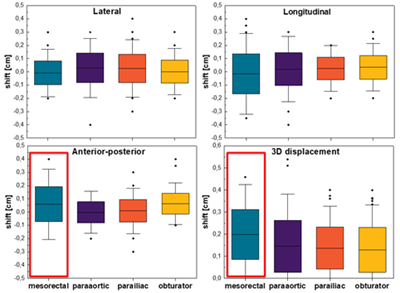
Figure 1 - Box-and-whisker plots (depicting the mean, 1SD, 2SD and outliers) of the intra-fraction displacement of lymph nodes for the different locations in the lateral, longitudinal and ant-post directions, as well as in 3D displacement
For isotropic PTV margins of 1mm, 2mm and 3mm, the percentage of fractions at which a node moved outside each of these margins is visualised in Figure 2 for the four localisations. For all but the mesorectal nodes, a 2mm margin ensured that the nodes remained inside the PTV for more than 90% of fractions during treatment. For the mesorectal nodes, a 3mm margin sufficed.
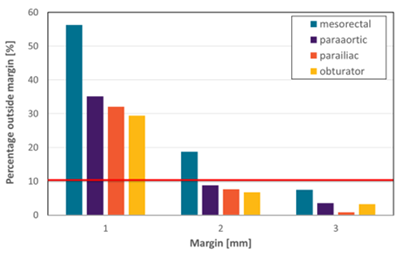
Figure 2 - Percentage of fractions in which the intra-fraction motion in one or more directions exceeds the PTV margin of 1, 2 and 3mm isotropically
Conclusion
Intrafraction motion of pelvic lymph nodes depends on their localisation. Lymph nodes located in the mesorectum show larger intra-fraction motion, compared with para-aortic, para-iliac and obturator nodes. A PTV margin of 3mm for the mesorectal nodes and 2mm for the other locations ensures that the target is inside the PTV for 90% of fractions.
My name is Mylène V. Noordeloos. I am a radiation therapist (RTT) at Radiotherapiegroep in The Netherlands. I conducted this research with my fellow RTTs Kim Antonissen and Karolin Ezendam, with the help of physicists and radiotherapy oncologists. Special thanks go to D. Schuring for his contributions.

For questions, you can contact me at: m.noordeloos@radiotherapiegroep.nl
Follow me on LinkedIn: Mylène Noordeloos
Follow us on Instagram and LinkedIn: Radiotherapiegroep